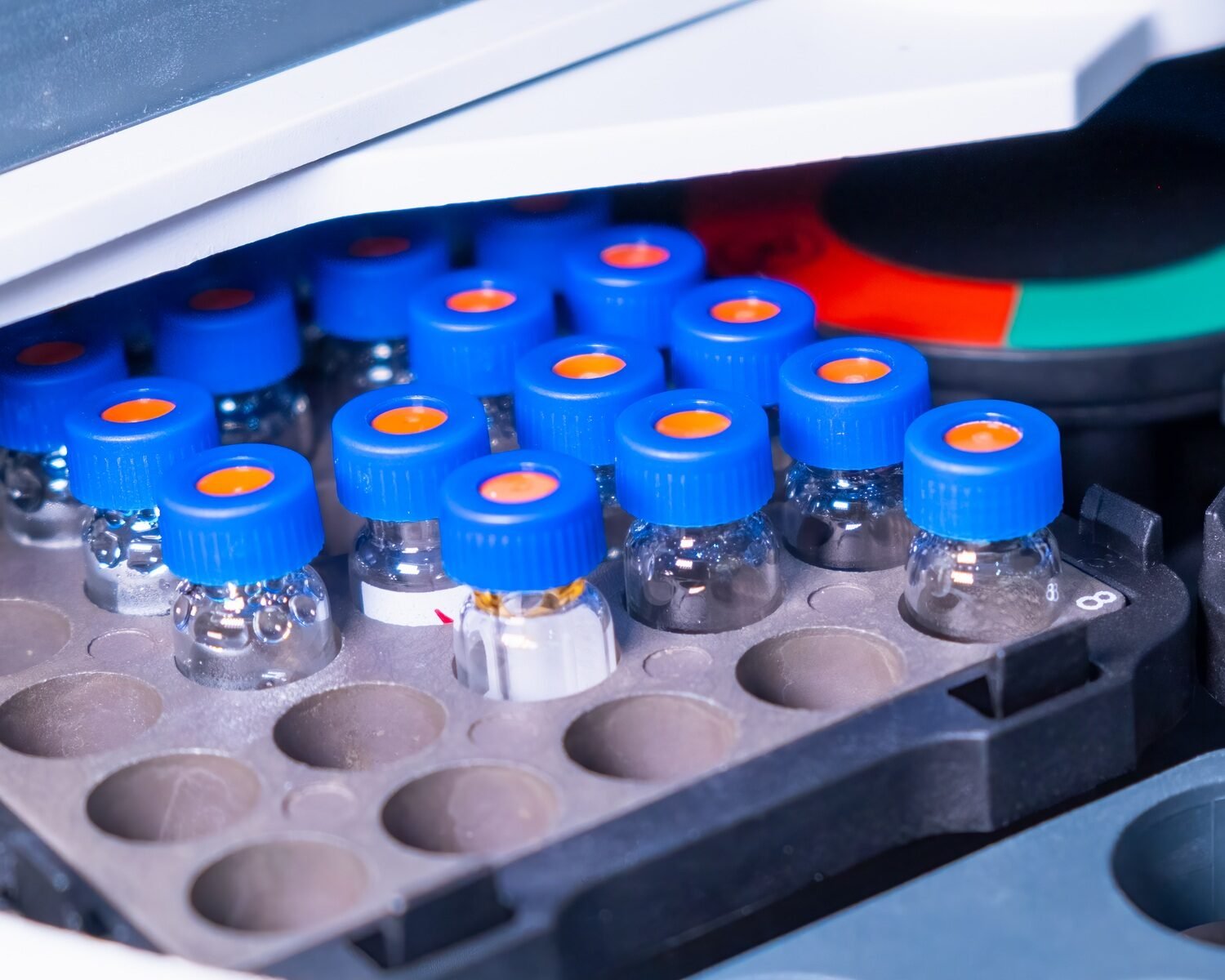
Innovations have advanced healthcare through the years. Technologies are not only prolonging but also saving more lives. Science has made it possible to detect disease and avoid it through genetic screening and gene therapy. Laboratories can put HPLC to use to analyze one’s blood for the diagnosis of medical conditions. One of those is thalassemia, which affects millions of people worldwide. Physicians can advise corrective measures. Preparation can improve life outcomes with just a blood sample from the parents or the child.
I want to share with you in this article another wonder of HPLC in medical technology.
Importance of HPLC in Antenatal Care
Receiving antenatal care from a licensed physician during and after pregnancy is essential for the health of the mother and her baby. Unmonitored pregnancies can have serious consequences.
Screening for hemoglobinopathies
Hemoglobinopathies generally refer to any disorder that can be inherited. Hemoglobin’s abnormal production and structure characterize it. You might be familiar with sickle cells and thalassemia.
People have many types of hemoglobin, one of which is A2. Despite making up a tiny percentage of the blood, the variation level can help pinpoint certain conditions beyond hemoglobinopathies.
On the other hand, fetal hemoglobin can also be sampled through the unborn baby’s umbilical cord.
HPLC can be used to measure both A2 and fetal hemoglobin accurately.
Screening for thalassemias
Thalassemia is a genetic disorder affecting hemoglobin production that could lead to anemia. Almost every population carries a particular frequency of thalassemia. Anyone could be a carrier of the disorder even if they inherited it from just one of their parents. Worse, they can suffer from the condition if both parents are carriers. There is no way to prevent it unless you and your partner intentionally get screened for thalassemia before starting a family.
The adoption of CE-HPLC or cation-exchange HPLC to diagnose thalassemia has been rapid. The method is now used worldwide and can be used to detect all clinically significant variants of the disorder.
Food screening
The number of HPLC methods available to food analysts is growing. It is not as routinely used as gas chromatography, but HPLC offers a flexible platform for analyzing complex food matrices. It can be used to ensure the quality of food, especially for those pregnant who demand higher quality products in consideration of the baby.
Accurate and sensitive quantification of small concentrations of analytes ensures that no harmful compounds such as certain food colors make their way into your body.
What are thalassemias?
Thalassemia is a disorder that affects the way RBCs are formed. It can be inherited even if just one of the parents has the mutation. Whether you have a modified gene or some DNA fragments are missing from you, your body will produce an abnormal form of hemoglobin.
All humans have this protein in red blood cells. It gives your blood the appearance of being red, as it carries oxygen. The RBC or red blood cells naturally get “eaten” by the spleen and lymph nodes after 70 to 140 days. It is a form of quality control for your circulatory system as the RBCs mature and get some defects. People with the disorder will experience excessive destruction of the RBC. As the body destroys more RBC than is produced, the individual will also experience anemia.
Thalassemia can be either mild or severe. Some call it thalassemia and thalassemia minor. If you have thalassemia, your body does not make enough healthy red blood cells, which means you might be in for more health troubles.
Alpha vs. Beta-thalassemias
To tell alpha-thalassemia and beta-thalassemia apart, doctors can look at the red blood cells through a microscope. In people with alpha-thalassemia, the red blood cells have an unusual shape. They look smaller and rounder than usual. Therefore, they also don’t have enough room for the average amount of hemoglobin. Often, there are also small bursts on the surface of these abnormal-looking red blood cells.
Alpha-thalassemia is a condition passed down through families. The body makes fewer alpha-globin proteins than normal in individuals with the condition. Alpha-globin proteins make up two of the four subunits of every hemoglobin. One could have milder anemia, and symptoms are often not noticed until adulthood.
Some are not lucky enough when all four alpha gene regions are affected. It can cause severe complications in a developing fetus, such as poor growth and an enlarged liver and spleen. Affected pregnancies often do not come to term. This condition can be diagnosed before birth by amniocentesis or chorionic villus sampling. The second one can also be used to check for other genetic conditions.
Here are the four types of alpha-thalassemia that depend on the alpha-globin genes affected:
- Alpha-thalassemia silent carrier. You have smaller red blood cells because you either have three normal genes or four but with one damaged.
- Alpha-thalassemia carrier. You can be suffering from mild anemia because you only have 2 of the genes.
- Hemoglobin H disease. You only have one gene instead of the normal four. You may have moderate to severe anemia, but it can worsen if you have a fever or exposure to certain chemicals and medicines. You can have a child, though they can have thalassemia too.
- Alpha-thalassemia major. No normal genes were left. It is heartbreaking to know that the mother will likely experience a miscarriage.
On the other hand, beta-thalassemia involves HBB or hemoglobin beta gene mutations. To create normal amounts of hemoglobin, each cell must make four copies of the beta hemoglobin gene. Cells usually make 2 and 2 copies of beta hemoglobin. In people with beta-thalassemia, they only make 1 and 3 copies instead. This small change makes their bodies make fewer beta hemoglobin building blocks than usual.
People with beta-thalassemia tend to have more symptoms than people with alpha-thalassemia. Beta-thalassemia is much less common than alpha-thalassemia. The severity of beta-thalassemia mostly depends on how many copies of the beta hemoglobin gene are still working in a person’s body.
Here are two types of beta-thalassemia depending on the gene affected:
- Beta-thalassemia major. Two damaged genes cause this disorder, and individuals may get to live albeit shortly. It is also called Cooley’s anemia.
- Beta-thalassemia minor or thalassemia trait. One damaged gene causes less severe anemia, which can be passed to offspring with a 50 percent probability. It can be thalassemia minima characterized by minimal to no symptoms at all. Another is thalassemia intermedia, with moderate to severe anemia.
When do they manifest in affected individuals?
Persons with severe forms of thalassemia are more likely to get diagnosed with the disease in childhood. Though, the condition may be mistaken as a simple case of anemia. Persons with lesser forms of thalassemia may only find out because they have symptoms of anemia.
Another reason is that a doctor finds anemia on a routine blood test or a test done for another reason. If a relative has thalassemia, then you may have a variant too since you are related by blood. They can order tests for you to learn more about whether you might have it, too.
How early can they be detected?
In most cases, doctors diagnose thalassemia in children. This manifests in some individuals early in life where medical attention is focused. Doctors usually diagnose and treat these kids very early on. Other types of thalassemias may not be found until a kid develops mild or moderate anemia symptoms. Probably, it could be from a routine blood test with unusual results.
Then, if you’re pregnant or planning to be, you can talk with a genetic counselor about your child’s risk of having the condition. A screening test can show if you or your child carries the gene for thalassemia.
Is the condition life-threatening?
Yes, thalassemia can be life-threatening, although it is possible that an affected baby may not even reach childbirth. Thalassemia major is the most life-threatening form of beta-thalassemia. Symptoms of this disorder generally appear as the child turns two years of age.
Also, living with hemoglobin H and alpha-thalassemia major can sometimes feel like a burden. But having the condition doesn’t have to be that way. There are plenty of decisions you can make to guard your health and the health of the people you love. Early diagnosis by your physician is the key.
How HPLC helps in detecting the hemoglobin disorder
HPLC has been used in all aspects of the investigation of hemoglobinopathies. It ranges from identifying abnormal hemoglobin variants, detecting mutations, separation, and quantitation of globin chains to characterizing the structure by fingerprinting.
A comprehensive genetic investigation of abnormal hemoglobins is vital for a proper diagnosis and management of these disorders. Conventionally, an initial screening for abnormal hemoglobins using cellulose acetate electrophoresis was followed by a definitive confirmation using HPLC.
What compounds can be detected
HPLC can analyze proteins such as the hemoglobin itself, the peptides such as alpha and beta polypeptides, polyamines, and organic acids.
Methodology in using HPLC
CE-HPLC is widely used in laboratories worldwide to detect the variants of hemoglobins and check how much hemoglobin F and A2 are in the blood. The test will also work with newborn children, saving their lives and being healthy growing up.
HPLC machines for testing
HPLC has many machine specifications, but medical devices may cost more than your average machine. The technology is advanced, but it will keep on advancing.
Here are some of the HPLC machine models that can help a lot, but you can also contact suppliers:
Other diseases that can be screened by HPLC
Scientists will often take biological samples from existing sufferers for analysis when researching specific diseases and disorders. By looking at their blood samples under the microscope (literally and figuratively), researchers may identify signs of the disease and its progression. It can help them better treat future patients.
Cancers
Pancreatic cancer is a disease in dire need of better methods of detection. With HPLC, a team in Japan was able to detect early-stage pancreatic cancer using a simple blood test. Blood is essentially a mix of proteins, and HPLC can work with that.
Genetic disorders
HPLC can check for variations in DNA sequences with great accuracy and reliability. Its uses include mutational analysis, genotyping, LOH determination, and gene expression analysis. It can also help in gene research itself.
Heart diseases
True enough, HPLC can detect and characterize almost anything. Proteomic profile and enzyme levels can be gained from tissue samples, which means a more accurate diagnosis. Understanding disease at the molecular level means better doctors’ opinions and courses of treatment.
Alzheimer’s disease
Alzheimer’s disease is a neurologic disorder associated with aging. It is also the leading cause of dementia. Suppose HPLC is combined with tandem mass spectrometry. In that case, it can qualitatively and quantitatively analyze amyloid β peptides, which are related to the disease.
Diabetes
Hemoglobin A1C is a test used to check the blood sugar attached to the hemoglobin in the blood. HPLC has been used for the test until now, despite other available tests due to its accuracy. Methods that can be used include boronate affinity and ion exchange.
Conclusion
I know that many have known that HPLC can provide accurate and precise results. It has proven its importance in medical diagnoses and will continue to do so in the future. I would be eager to hear about scientific developments brought about by HPLC, especially in the medical community.
Mastelf aims to provide safe vials so that more people can run HPLC operations in safe position. Upon consultation, you can personally check our product catalog and receive a free sample.
Mastelf, with over 13 years of experience in chromatography vials, we can help you find the exact vials you need for your applications.


Our expertise ensures that you get reliable and precise products tailored to your specific requirements. Whether you’re in pharmaceuticals, research, or any other industry relying on HPLC, we understand your needs and are here to support you in making the right purchase.
Reach out to Mastelf, and let us assist you in procuring the perfect vials for your work.